At first glance, the healthcare patient check-in process seems straightforward. But when examined through the lens of your revenue cycle and patient experience, it’s one of the most important interactions for your team to get right.
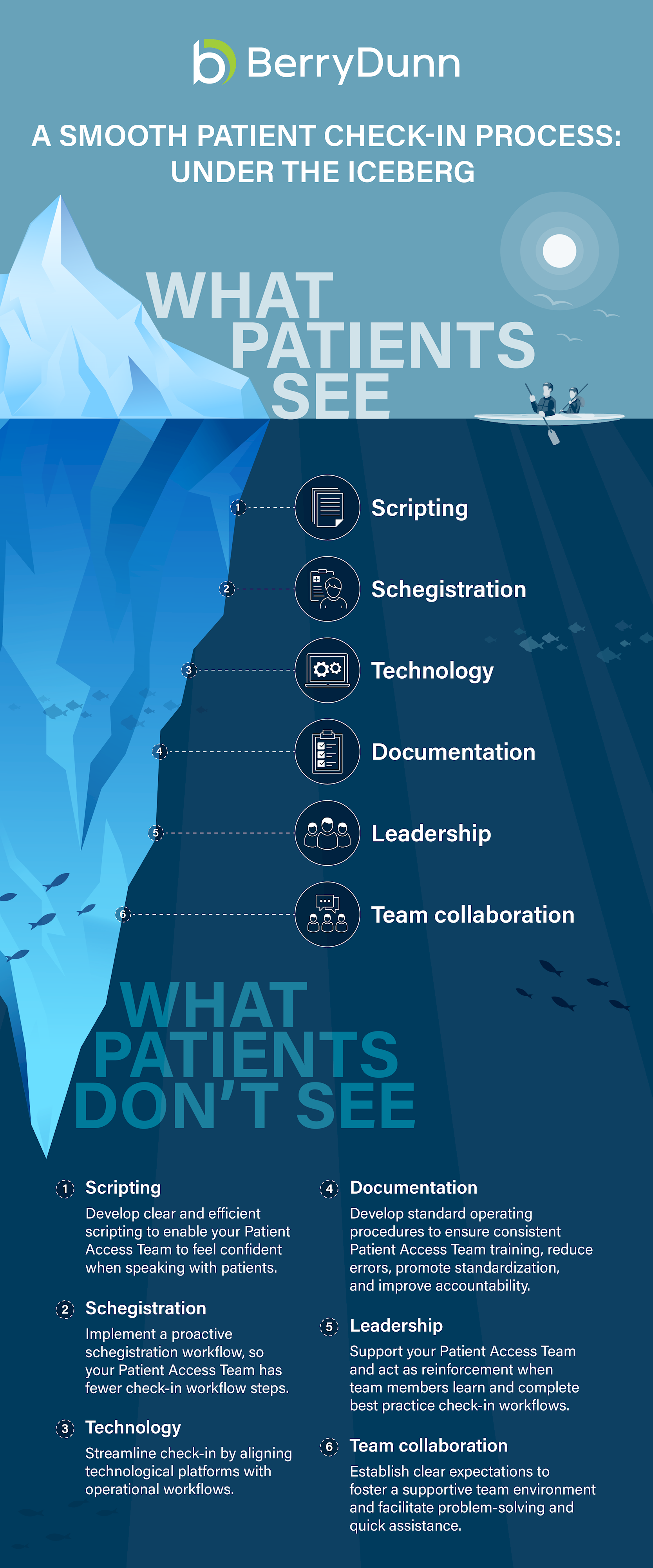
Several key elements must be taken into consideration to create a smooth and simple patient check-in. Patient satisfaction is the tip of the iceberg. You want your patients to have a great experience that is efficient, easy-to-understand, and doesn’t create billing headaches for them later on. The good news is that the same techniques that give your patients a good experience also form the basis for an optimal revenue cycle. Developing this process starts with the undersurface elements that patients never see.
Scripting for patient access teams
Communicating clearly, consistently, and positively is important to put patients at ease, and to make sure that you collect the most accurate and up-to-date information from patients. Doing this correctly up front will save time and will prevent denials and associated workload and revenue loss. The best practice is to establish scripting for your patient access staff and provide training to make sure they are confident in the scripting provided. Here are some examples:
When confirming that patient information is up to date:
Say this: “To ensure your account is as accurate as possible, we require all patients to present a minimum amount of information.”
Not that: “Have there been any changes in your information since the last time you were here?”
Or when connecting a self-pay patient with a financial counselor:
Say this: “Before scheduling your appointment, I will connect with a financial counselor who can determine if you qualify for assistance and will help you understand your financial obligations.”
Not that: “We can’t schedule you until you speak with someone in Finance.”
Developing clear and efficient scripting will give your team the tools to communicate effectively and will help your patients feel like they are well taken care of.
Schegistration: What is it?
What is “schegistration” anyway? Schegistration is the process of scheduling a patient appointment while also pre-registering the patient at the same time. By gathering and confirming information at the time of scheduling, the in-person check-in process will have fewer steps and will be quicker and easier for both the patient and your team.
Technology: Align your EHR with patient access workflows
Technology, specifically your Electronic Health Record (EHR), can either make your workflows more efficient, or can hinder your patient access staff. It’s important to align your technology platforms with your operational workflows, so it is seamless for your staff to enter and pull up information. It’s also important to have your staff trained regularly on your technology systems so they feel confident that they are using the system correctly and most efficiently.
Documentation: Write it down!
When you develop new workflows to increase efficiency and the patient experience, it can be challenging for staff to make the change. In a busy office environment, it can also be difficult to train new staff effectively. To make it easy and to create consistency and continuity, it’s important to develop standard operating procedures and to document them thoroughly. Providing easy to understand instructions, including visuals of workflows, will reduce errors, promote standardization, and improve accountability.
Leadership: Reinforce best practice workflows
Keeping workflows optimized takes the whole team, beginning with leadership. The leaders of your patient access team should act as reinforcement when team members learn and complete best practice check-in workflows. Having documentation readily available and providing support and encouragement to team members will help keep your processes running smoothly.
Patient access team collaboration
Establish clear expectations to foster a supportive team environment and facilitate problem-solving and quick assistance. When scripting, workflows, and documentation are consistent, it’s easy for team members to help each other out and support each other when challenges arise.
The healthcare revenue cycle is an intricate system involving interdependent functions. Like an ecosystem, each component plays an important role in the system. The patient access process is just one piece of the puzzle. Optimizing your revenue cycle also includes looking at these areas: coding and compliance, billing, and denial management.
BerryDunn's audit, tax, clinical, and consulting professionals, focused on specific healthcare industry areas, understand the biggest challenges facing healthcare leaders, and are committed to helping you meet and exceed regulatory requirements, maximize your revenue, minimize your risk, improve your operations—and most importantly—facilitate positive outcomes. Learn more about our healthcare consulting team.