What the C-Suite should know about CECL and change management
Read this if you are at a financial institution.
Some institutions are managing CECL implementation as a significant enterprise project, while others have assigned it to just one or two people. While these approaches may yield technical compliance, leadership may find they fail to realize any strategic benefits. In this article, Dan Vogt, Principal in BerryDunn’s Management and IT Consulting Practice, and Susan Weber, Senior Manager and CECL expert in BerryDunn’s Financial Services Practice, outline key actions leaders can take now to ensure CECL adoption success.
Call it empathy, or just the need to take a break from the tactical and check in on the human experience, but on a recent call, I paused the typical readiness questions to ask, “How’s the mood around CECL adoption – what’s it been like getting others in the organization involved?” The three-word reply was simple, but powerful: “Kicking and screaming.”
Earlier this year, by a vote of 5-2, the FASB (Financial Accounting Standards Board) closed the door to any further delays to CECL adoption, citing an overarching need to unify the industry under one standard. FASB’s decision also mercifully ended the on-again off-again cycle that has characterized CECL preparation efforts since early 2020. One might think the decision would have resulted in relief. But with so much change in the world over the past few years, is it any wonder institutions are instead feeling change-saturated?
Organizational change
CECL has been heralded as the most significant change to bank accounting ever, replacing 40+ years of accounting and regulatory oversight practices. But the new standard does much more than that. Implementing CECL has an effect on everything from executive and board strategic discussions to interdepartmental workflows, systems, and controls. The introduction of new methods, data elements, and financial assets has helped usher in new software, processes, and responsibilities that directly affect the work of many people in the organization. CECL isn’t just accounting—it’s organizational change.
Change management
Change management best practices often focus on leading from optimism—typically leadership and an executive sponsor talk about opportunities and the business reasons for change. Some examples of what this might sound like as it relates to CECL might include, by converting to lifetime loss expectations, the institution will be better prepared to weather economic downturns; or, by evolving data and modeling precision, an institution’s understanding and measure of credit risk is enhanced, resulting in more strategic growth, pricing, and risk management.
But leading from optimism is sometimes hard to do because it isn’t always motivating—especially when the change is mandated rather than chosen.
Perhaps a more judiciously used tactic is to focus on the risk, or potential penalty, of not changing. In the case of CECL, examples might include, your external auditor not being able to sign-off on your financials (or significant delays in doing so), regulatory criticism, inefficient/ineffective processes, control issues, tired and frustrated staff. These examples expose the institution to all kinds of key risks: compliance, operational, strategic, and reputational, among them.
CECL success and change management
With so much riding on CECL implementation and adoption going well, some organizations may be at heightened risk simply because the effort is being compartmentalized—isolated within a department, or assigned to only one or two people. How effectively leadership connects CECL implementation with tenets of change management, how quickly they understand, then together embrace, promote, and facilitate the related changes affecting people and their work, may prove to be the key factor in achieving success beyond compliance.
One important step leaders can take is to perform an impact assessment to understand who in the organization is being affected by the transition to CECL, and how. An example of this is below. Identifying the departments and functions that will need to be changed or updated with CECL adoption might expose critical overlaps and reveal important new or enhanced collaborations. Adding in the number of people represented by each group gives leaders insight into the extent of the impact across the institution. By better understanding how these different groups are affected, leaders can work together to more effectively prioritize, identify and remove roadblocks, and support peoples’ efforts longer term.
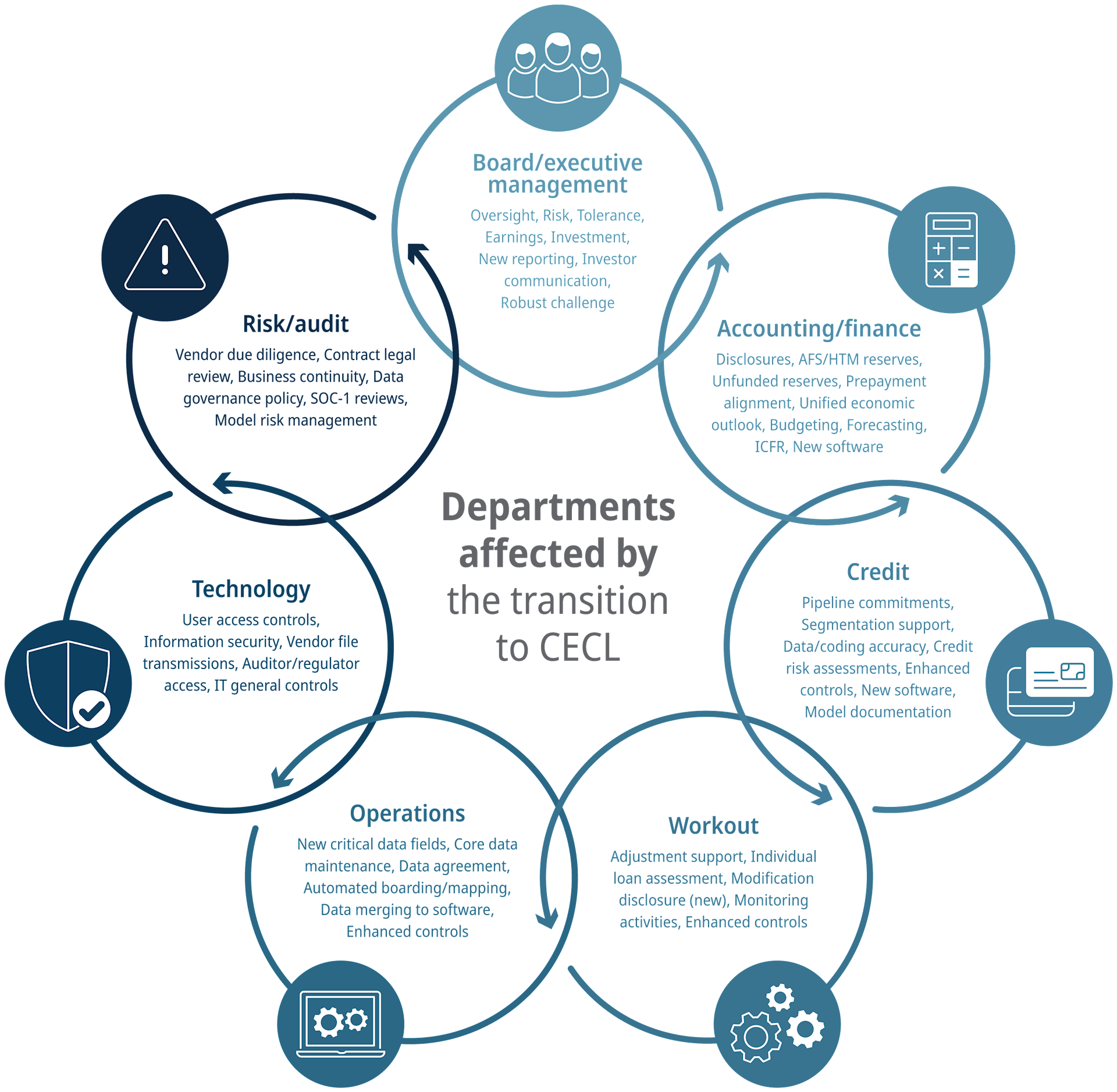
No matter where your institution is currently in its CECL implementation journey, it is not too late to course-correct. Leadership—unified in priority, message, and understanding—can achieve the type of success that produces efficient sustainable practices, and increases employee resilience and engagement.
For more information, visit the CECL page on our website. If you would like specific answers to questions about your CECL implementation, please visit our Ask the Advisor page to submit your questions. For more tips on documenting your CECL adoption, stay tuned for our next article in the series, revisit past articles, or tune in to our CECL Radio podcast. You can also follow Susan Weber on LinkedIn.